TL;DR:
- Primary care provides essential ongoing management and coordination for chronic conditions.
- Medicare covers services like APCM and CCM to enhance primary care access and coordination.
- Understanding and utilizing these programs can improve health outcomes and reduce costs.
Many Medicare beneficiaries focus on hospital visits and specialist appointments, assuming those are the most important parts of their coverage. But here's what often gets missed: primary care is the foundation that keeps everything else working well. It's the layer of care that catches problems early, coordinates your treatments, and helps you manage conditions like diabetes, heart disease, or high blood pressure before they become emergencies. For Medicare enrollees in North Bergen and Secaucus, understanding how primary care fits into your coverage can make a real difference in your health and your costs. This article breaks down what Medicare actually covers, how programs like Chronic Care Management work, and what you can do to get more from your plan.
Table of Contents
- Why primary care matters in Medicare
- How Medicare covers primary care services
- Chronic care management: A Medicare primary care advantage
- Overcoming barriers: Utilization, payment, and policy reforms
- A local perspective: What most Medicare guides miss about primary care
- Take the next step: Comprehensive primary care with local experts
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Primary care is foundational | Access to strong primary care is key to better health outcomes and cost savings for Medicare beneficiaries. |
| Comprehensive coverage options | Medicare includes a range of primary care services, with new models like APCM and CCM offering more coordination and 24/7 support. |
| Chronic care needs attention | Chronic Care Management is essential for those with multiple conditions but is underused, so eligible beneficiaries should ask about it. |
| Advocacy impacts reform | Understanding and supporting Medicare policy reforms can improve access and quality of primary care for everyone. |
Why primary care matters in Medicare
Primary care is the ongoing relationship you have with a physician, nurse practitioner, or physician assistant who knows your full health picture. It's not just about treating a cold or getting a prescription refilled. It's about managing your overall health over time, tracking changes, and coordinating care across specialists and hospitals. For Medicare beneficiaries, that kind of continuity is especially important.
Many people with Medicare are managing more than one chronic condition. Heart disease, diabetes, arthritis, and chronic lung conditions are common. Without a primary care provider coordinating everything, it's easy for treatments to conflict, for follow-ups to fall through the cracks, or for a manageable condition to worsen unnecessarily. Primary care is the layer of the healthcare system that prevents those gaps.
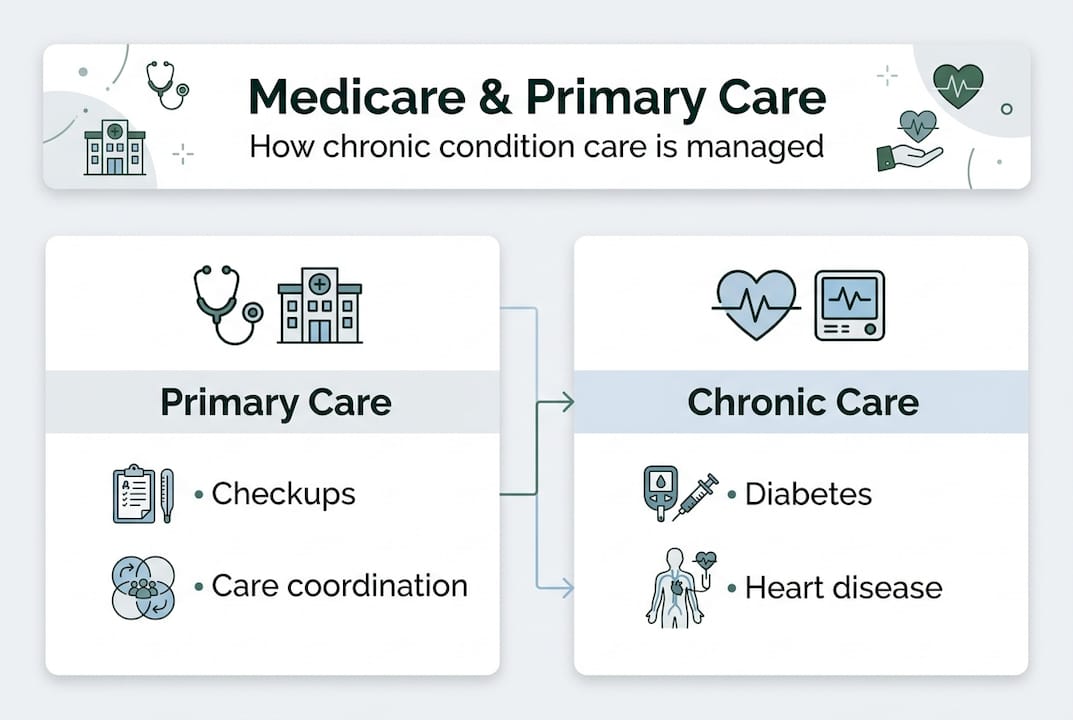
Despite this, Medicare has historically underinvested in primary care, spending only 5 to 8% on it compared to 13% among peer health systems. That gap has real consequences for patients who need consistent, coordinated care.
Here's what primary care actually does for you as a Medicare beneficiary:
- Detects health problems early through regular checkups and screenings
- Manages chronic conditions with ongoing monitoring and treatment adjustments
- Coordinates care between specialists, labs, and hospitals
- Reduces unnecessary emergency room visits
- Supports medication management and adherence
- Provides preventive care to lower long-term health risks
Policy experts argue that strengthening primary care in Medicare directly addresses the 90% of Medicare spending driven by chronic disease. Investing in primary care isn't just good medicine. It's smart policy.
For a broader look at your primary care service options, it helps to understand exactly what Medicare makes available to you.
How Medicare covers primary care services
Medicare Part B is the part of your coverage that handles outpatient services, and that includes primary care. Under Part B, you have access to preventive services, annual wellness visits, and ongoing care for chronic conditions. But Medicare has also expanded what's available through a program called Advanced Primary Care Management, or APCM.
APCM is a newer Medicare benefit designed to strengthen the primary care relationship. Medicare covers APCM under Part B, providing 24/7 access to your care team, chronic care management, personalized care plans, care coordination, transitional care after hospitalizations, and medication management. These aren't just add-ons. They're structured services that make your primary care more responsive and proactive.
Here's a summary of key services covered under Medicare's primary care framework:
| Service | What it includes |
|---|---|
| Annual wellness visit | Health risk assessment, preventive planning |
| 24/7 care access | After-hours contact with your care team |
| Personalized care plan | Written plan tailored to your conditions |
| Care coordination | Communication between providers |
| Transitional care | Support after hospital discharge |
| Medication management | Review and reconciliation of all medications |
To get started with APCM, the process is straightforward:
- Schedule an initiation visit with your primary care provider to discuss APCM enrollment.
- Provide verbal or written consent to participate in the program.
- Work with your provider to develop a personalized care plan.
- Confirm your coinsurance responsibility (typically 20% after the Part B deductible).
- Begin receiving coordinated care services, including between-visit support.
If you're unsure about your Medicare insurance options or want to explore available care management programs, speaking with a local provider is a good first step. You can also review Medicare coverage explained for more detail on what applies in New Jersey.

Pro Tip: Keep all your medical records, medication lists, and prior visit summaries organized in one place. This makes it much easier to transition between programs or providers without losing important health history.
Chronic care management: A Medicare primary care advantage
If you have two or more chronic conditions, Medicare offers a specific benefit called Chronic Care Management, or CCM. This is one of the most valuable and underused tools available to Medicare beneficiaries, and it goes well beyond a standard office visit.
CCM is a monthly Medicare service for patients with two or more chronic conditions, covering non-face-to-face care coordination, between-visit medical support, and ongoing medication management. Your care team works on your behalf even when you're not in the office, checking in, coordinating with specialists, and making sure your care plan stays current.
Here's how CCM compares to standard primary care:
| Feature | Standard primary care | With CCM |
|---|---|---|
| Care coordination | During visits only | Ongoing, between visits |
| Care plan | Informal or verbal | Written, updated regularly |
| After-hours access | Limited | 24/7 contact available |
| Medication review | At appointments | Continuous reconciliation |
| Specialist communication | Patient-managed | Provider-to-provider |
Despite these clear benefits, CCM utilization remains low, rising from just 1.1% to 3.4% of eligible beneficiaries between 2015 and 2019, reaching 1.3 million in 2023 with 23% year-over-year growth. Still, only 77% of CCM claims had two or more chronic conditions properly documented.
The benefits for patients who do use CCM are significant:
- Fewer emergency room visits and hospitalizations
- Better medication adherence and fewer dangerous interactions
- More consistent follow-up on test results and referrals
- A care team that knows your full history, not just your last visit
- Reduced stress from managing complex conditions alone
You can learn more about enrolling in a local CCM program, review CCM FAQs, or read about how CCM improves health outcomes over time.
Pro Tip: Make sure your provider has documented all your chronic conditions in your medical record. Incomplete documentation is one of the main reasons patients miss out on CCM eligibility.
Overcoming barriers: Utilization, payment, and policy reforms
Even with strong programs like APCM and CCM available, many Medicare beneficiaries still don't access them. The reasons are a mix of awareness gaps, administrative hurdles, and how Medicare currently pays for primary care.
The core problem is structural. Medicare has historically undervalued primary care coordination, with spending at 5 to 8% compared to 13% among peer systems. This creates pressure on primary care practices to see more patients in less time, which makes it harder to offer the kind of thorough, coordinated care that Medicare beneficiaries with chronic conditions actually need.
For patients, the barriers often look like this:
- Not knowing that programs like CCM or APCM exist
- Providers not offering enrollment due to administrative complexity
- Difficulty navigating the consent and documentation requirements
- Coinsurance costs creating hesitation, even when savings are significant
- Fragmented care between specialists and primary care providers
The good news is that reform efforts are gaining momentum. Health policy experts recommend increasing Part B resources dedicated to primary care, expanding Alternative Payment Model bonuses for practices that deliver coordinated chronic care, and reducing administrative burdens that discourage providers from offering CCM.
CCM has been shown to reduce emergency department visits by an average of $888 per beneficiary per year. Low uptake due to administrative burdens and enrollment gaps means many patients are leaving real savings and better care on the table. APCM helps ease this by removing time-logging requirements.
As a Medicare beneficiary in North Bergen or Secaucus, you don't have to wait for policy changes to benefit. Understanding primary care and health outcomes and applying tips for managing chronic conditions can help you take full advantage of what's already available to you.
A local perspective: What most Medicare guides miss about primary care
Most Medicare guides give you a list of covered services and stop there. What they don't tell you is that the quality of your primary care relationship matters just as much as what's technically covered. In North Bergen and Secaucus, where many residents are managing multiple chronic conditions, having a provider who truly knows your history makes a measurable difference.
We've seen patients who visited specialists for years without anyone coordinating the full picture. When they established a consistent primary care relationship and enrolled in CCM, their outcomes improved, their medication lists got cleaner, and their ER visits dropped. That's not a coincidence.
What most people miss is the value of 24/7 access and real care coordination. It's not about calling your doctor at midnight for minor issues. It's about having a system in place so that when something changes, someone is paying attention.
The practical step is simple. Review all your chronic conditions and current medications with your primary care provider at your next annual visit. Ask directly about APCM or CCM eligibility. Bring a family member if it helps. And choose a provider who treats your ongoing care as a priority, not just your acute symptoms.
For help choosing the right primary care provider in Hudson County, start by looking for a practice that offers coordinated chronic care programs.
Take the next step: Comprehensive primary care with local experts
Armed with these insights, here's how you can put them into action with local providers.
At Garden State Medical Group, we work with Medicare beneficiaries in North Bergen and Secaucus to make sure they're getting the full benefit of their coverage. Our primary care services include coordinated care for chronic conditions, annual wellness visits, and enrollment support for programs like CCM.
If you're managing diabetes, heart disease, or any other ongoing condition, our chronic care management program is designed to keep you supported between visits, not just during them. We also offer a full range of programs tailored to your specific health needs. Contact us today to schedule a visit and find out which Medicare primary care programs are right for you.
Frequently asked questions
What does primary care mean in Medicare?
Primary care in Medicare refers to general healthcare services like routine checkups, preventive care, care coordination, and managing chronic conditions provided by a physician, nurse practitioner, or PA. Medicare Part B covers these services, including expanded options like APCM that provide 24/7 access and personalized care plans.
Who is eligible for Chronic Care Management under Medicare?
Medicare beneficiaries with two or more chronic conditions expected to last at least twelve months or until death qualify for CCM services. Your provider must document those conditions and obtain your consent before billing for CCM.
What is the cost of primary care services under Medicare?
After the Part B deductible, Medicare typically pays 80% of approved primary care services, leaving you responsible for 20% coinsurance. Beneficiaries who are dually eligible for Medicaid often pay $0 for these services.
Can I use both APCM and CCM in the same month?
No, Medicare does not allow billing APCM and CCM for the same patient in the same month. Your provider will help determine which program better fits your current care needs.
